Non-Puerperal Uterine Inversion Caused by a Submucosal Leiomyoma: A Rare Case Report
Received Date: November 16, 2025 Accepted Date: December 06, 2025 Published Date: December 10, 2025
doi:10.17303/jwhg.2025.12.204
Citation: Ouafa Guellati (2025) Non-Puerperal Uterine Inversion Caused by a Submucosal Leiomyoma: A Rare Case Report. J Womens Health Gyn 12: 1-7
Abstract
Background: Non-puerperal uterine inversion is an exceptionally rare gynecological complication, most often secondary to an intracavitary uterine tumor, particularly a submucosal fibroid. Its non-specific clinical presentation, combining abnormal genital bleeding, pelvic pain and a vaginal mass, may lead to delayed diagnosis and suboptimal management, especially in women of reproductive age.
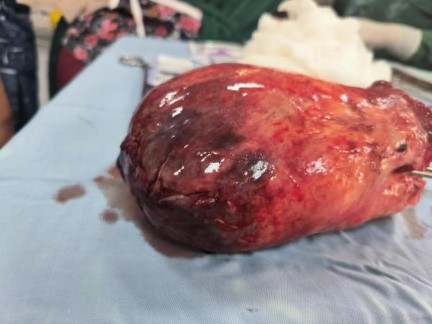
Case Presentation: We report the case of a 35-year-old nulliparous, unmarried woman admitted with a two-day history of pelvic pain and vaginal bleeding, associated with severe anemia (hemoglobin 7 g/dL). Speculum examination revealed a pedunculated mass of approximately 10 cm prolapsing into the vagina, while the uterus was not palpable in its usual suprapubic position. Pelvic ultrasound showed an enlarged uterus with a submucosal fibroid displacing the endometrium, without adnexal abnormalities. After transfusion of two units of packed red blood cells, an abdominal myomectomy was scheduled. Intraoperative findings revealed a non-puerperal uterine inversion, confirmed by a depressed and invaginated uterine fundus. An anterior incision at the constriction ring allowed enucleation of the fundal fibroid and reconstruction of the uterine fundus. The gross specimen of the leiomyoma is shown in Figure 1. Histopathological examination concluded to a benign submucosal leiomyoma. Postoperative course was uneventful, with resolution of the bleeding and progressive correction of anemia.
Discussion: This case highlights the diagnostic challenge of non-puerperal uterine inversion, which can mimic an expelled fibroid or genital prolapse. The association of a large vaginal mass with a non-palpable uterus should raise suspicion of uterine inversion and prompt appropriate imaging and surgical exploration. In young women with benign disease, an abdominal approach can confirm the diagnosis, treat the causative lesion, and allow uterine-sparing management.
Conclusion: Non-puerperal uterine inversion secondary to a submucosal fibroid is rare but should be considered in the differential diagnosis of a vaginal mass with an absent or difficult-to-palpate uterus. Early suspicion and individualized surgical strategy can correct the inversion while preserving the uterus in women of reproductive age.
Keywords: Non-Puerperal Uterine Inversion; Submucosal Fibroid; Leiomyoma; Abnormal Uterine Bleeding; Abdominal Myomectomy
Introduction
Uterine inversion is a rare condition defined by invagination of the uterine fundus into the uterine cavity, which may progress to complete externalization of the uterine body into the vagina [1-4]. It most commonly occurs in the obstetrical setting, during or immediately after delivery, where it constitutes a life-threatening emergency because of massive hemorrhage and shock [1, 2]. Outside the postpartum period, so-called non-puerperal uterine inversion is an exceptional entity, accounting for only a small fraction of all uterine inversions reported in the literature [1-4].
Non-puerperal forms are most frequently associated with an underlying uterine tumor, benign or malignant, acting as a triggering factor through traction on the uterine fundus [1-4]. Among these etiologies, submucosal fibroids occupy a prominent place. Located in contact with the endometrium, sometimes pedunculated and bulky, they may progressively prolapse through the cervix and, by traction and invagination, lead to inversion of the uterine body [5-9]. This situation nevertheless remains exceptional and is reported mainly as isolated case reports or small series [2, 3, 5-12].
Clinically, non-puerperal uterine inversion most often presents with chronic or acute abnormal uterine bleeding, pelvic pain and the appearance of a vaginal mass [2, 3, 5-12]. This non-specific picture frequently leads to confusion with more common conditions such as an expelled fibroid or polyp, genital prolapse, or cervical or endometrial tumors [2, 3, 5-12]. Abdominal palpation may reveal a uterus that is difficult to identify or absent from its usual position, but this sign is not always recognized [2, 3, 5-12]. Imaging, particularly pelvic ultrasound and, when available, magnetic resonance imaging (MRI), can contribute to the diagnosis by suggesting inversion; the characteristic MRI signs have been well described and confirmed in several series [4, 13, 14]. However, in many cases, the definitive diagnosis is only made intraoperatively [2, 3, 5-12].
This rarity, combined with a deceptive clinical presentation, exposes patients to diagnostic delays and initially inappropriate therapeutic decisions, particularly in women of reproductive age for whom fertility preservation is a major issue [2, 3, 5-12]. The aim of this report is to describe a case of non-puerperal uterine inversion secondary to a submucosal fibroid and to discuss its diagnostic and therapeutic particularities in the light of the literature [1-15].
Case Report
A 35-year-old unmarried woman, with no recent obstetric history, was admitted to our department with pelvic pain and vaginal bleeding evolving over two days, with marked exacerbation on the day of admission.
On general examination, her hemodynamic status was stable. Abdominal examination revealed a soft abdomen without guarding or localized tenderness. Speculum examination showed a circular pedunculated mass of approximately 10 cm in diameter prolapsing into the vagina and descending further with the Valsalva maneuver. Bimanual examination revealed a mass occupying the entire vaginal space with a thick base, while the uterus was not palpable in its usual suprapubic position.
Transabdominal and transvaginal pelvic ultrasound demonstrated a submucosal fibroid measuring 10 × 72 mm, displacing the endometrium, and an overall enlarged uterus measuring 86 × 99 × 109 mm, with no adnexal abnormalities. Initial laboratory investigations revealed severe anemia, with hemoglobin at 7 g/dL and hematocrit at 24%, consistent with the marked clinical pallor. The patient received two units of packed red blood cells preoperatively and was subsequently prepared for an abdominal myomectomy.
In the operating room, after induction of general anesthesia, a suprapubic laparotomy was performed. Intraoperative exploration showed an invaginated uterus with a depressed fundus pulled downward, an appearance highly suggestive of non-puerperal uterine inversion. Correlation with clinical findings (non-palpable uterus on abdominal examination and pedunculated vaginal mass) confirmed the diagnosis.
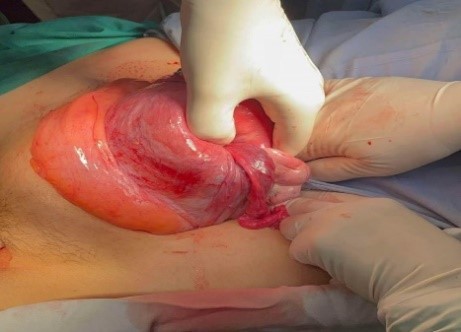
An anterior incision was made at the level of the constriction ring via the abdominal approach, allowing careful enucleation of the fibroid inserted at the uterine fundus. The gross specimen of the leiomyoma is depicted in Figure 1. The inverted uterine fundus was then restored to its normal position. The underlying endometrium and myometrium were meticulously repaired using 2-0 chromic absorbable sutures, thereby restoring the integrity of the uterine cavity. An intraoperative view of the inverted uterus being managed through the laparotomy is shown in Figure 2.
The surgical specimen was sent for histopathological examination, which confirmed a benign submucosal uterine leiomyoma with no evidence of malignancy.
The postoperative course was favorable. The patient experienced neither hemorrhagic nor infectious complications. Clinical improvement was rapid, with resolution of pelvic pain and cessation of abnormal bleeding. Postoperative laboratory tests showed progressive correction of anemia. At follow-up, gynecological examination revealed a normally sized uterus, in normal position, with no residual vaginal mass. The patient reported no further episodes of metrorrhagia or pelvic symptoms.
Discussion
Non-puerperal uterine inversion is a distinct entity compared to puerperal forms, which account for the vast majority of uterine inversions [1-4]. The systematic review by Rosa Silva et al. confirmed that non-puerperal inversions represent only a small proportion of published cases and are most often secondary to an intracavitary uterine tumor, either benign or malignant [1]. Among these etiologies, a fundal submucosal leiomyoma, particularly when pedunculated and voluminous, is the most frequently reported cause [5-9]. The fibroid exerts traction on the uterine fundus as it progresses through the cervix, favoring invagination and ultimately inversion of the uterine body [5-9].
The present case fits this classic etiologic framework of non-puerperal uterine inversion secondary to a submucosal fibroid, in line with numerous case reports and series published in recent years [2, 3, 5-12].
From a clinical standpoint, the most frequently reported manifestations include abnormal uterine bleeding, often leading to anemia, pelvic pain and the presence of a vaginal mass [2, 3, 5-12]. Our patient presented this typical triad, with recent pelvic pain, acute vaginal bleeding and severe anemia, associated with a large pedunculated vaginal mass. However, this clinical picture is non-specific. In the literature, non-puerperal uterine inversion is often misdiagnosed as an expelled fibroid or polyp, genital prolapse, or cervical or endometrial malignancy [2, 3, 5-12]. Many authors emphasize that the diagnosis is often made intraoperatively, under the initial assumption of an isolated pedunculated uterine tumor [2, 3, 5-12].
An important but sometimes overlooked clinical sign is the absence of the uterus in its usual position on abdominal and bimanual examination when a mass occupies the vagina [2, 3, 5-12]. In our case, the combination of a thick-based vaginal mass and a non-palpable uterus was present and prompted suspicion of underlying inversion. This underscores the value of a meticulous physical examination in avoiding diagnostic delay.
Imaging plays a key role in diagnostic orientation. Pelvic ultrasound is the first-line examination and may reveal an enlarged, poorly defined uterus associated with an intracavitary or intravaginal mass [1-4, 13, 14]. However, sonographic signs are often indirect. MRI, when available, provides more specific findings: a U-shaped uterine cavity, thickened and invaginated uterine fundus on sagittal views, and a “target” or “bull’s eye” appearance on axial sections [4, 13, 14]. These signs were initially described by Lewin and Bryan and subsequently confirmed by other teams [4, 13, 14]. In our observation, ultrasound documented a large submucosal fibroid and uterine enlargement, but was insufficient by itself to establish the diagnosis of inversion, which is consistent with published data showing that the definitive diagnosis frequently remains intraoperative [2,3,5-12].
There is no standardized consensus regarding the optimal management of non-puerperal uterine inversion. The choice of surgical approach and the extent of the procedure depend on the patient’s age, reproductive desires, degree of inversion, tumor size and the suspected benign or malignant nature of the lesion [1-3, 6, 7, 12, 15]. The systematic review by Rosa Silva et al. reported that hysterectomy is the most frequently chosen treatment, particularly in postmenopausal women or when malignancy is suspected [1]. In this context, several authors have described abdominal procedures (e.g. Haultain or Huntington techniques) involving incision of the constriction ring and reduction of the inversion, followed by hysterectomy or myomectomy [1-3, 6, 7, 12, 15]. Other teams have reported vaginal approaches, especially in older patients with highly prolapsed masses, sometimes using techniques such as that described by Spinelli [2, 7]. Combined or minimally invasive approaches (laparoscopy associated with a vaginal step) have also been reported with good results [2, 6, 15].
In our case, given the patient’s young age, the strong suspicion of a benign lesion and the presence of severe anemia requiring optimal control of hemostasis, an abdominal approach was chosen. Laparotomy allowed confirmation of the inversion, performance of an anterior incision at the constriction ring, enucleation of the fundal fibroid at its implantation site and subsequent reconstruction of the uterine fundus. This conservative strategy is consistent with several published cases in which myomectomy combined with correction of the inversion was performed in young women, with preservation of the uterus [2, 3, 5-9, 11, 12].
Our observation has several noteworthy features: the occurrence of non-puerperal uterine inversion in a young woman outside any obstetrical context; presentation as a large pedunculated vaginal mass associated with severe anemia, mimicking an isolated expelled fibroid; the decisive role of clinical examination (non-palpable uterus, thick pedicle) in raising early suspicion of inversion; and conservative management via an abdominal approach with myomectomy and fundal reconstruction, thereby avoiding hysterectomy. In line with recent series emphasizing the diagnostic challenges and the importance of uterine preservation in young patients [2, 3, 10-12], this case underlines the need to consider non-puerperal uterine inversion in the differential diagnosis of any large vaginal mass associated with a difficult-to-palpate uterus and to adopt an individualized surgical strategy.
Conclusion
Non-puerperal uterine inversion of myomatous origin is an exceptional complication whose diagnosis relies primarily on recognition of simple clinical signs: pedunculated vaginal mass, abnormal bleeding and a uterus that is absent or difficult to palpate in its usual position. Our observation shows that early suspicion, supported by imaging and confirmed intraoperatively, guides appropriate therapeutic decision-making.
In the present case, abdominal management with myomectomy and uterine fundus reconstruction corrected the inversion while preserving the uterus in a young patient, with a favorable clinical outcome. This case emphasizes the importance of an individualized approach that considers patient age, fertility desires and the benign nature of the lesion, in order to avoid systematic resort to hysterectomy and to optimize functional prognosis in women presenting with non-puerperal uterine inversion secondary to a submucosal fibroid.
- Rosa Silva B, de Oliveira Meller F, Uggioni ML (2018) Non-puerperal uterine inversion: a systematic review. Gynecol Obstet Invest. 83: 428-36.
- Sasotya RS, Wu L, Lin X (2024) Diagnostics and management challenges of nonpuerperal uterine inversions: a case series. Int J Womens Health. 16:1425-35.
- Shasindran R, Dharshini N, Aruku N (2024) Exploring non-puerperal uterine inversion: a case series. Cureus. 16: e53071.
- Leconte I, Thierry C, Bongiorno A, Luyckx M, Fellah L (2016) Non-puerperal uterine inversion. J Belg Soc Radiol. 100: 47.
- Alsahabi J (2019) Non-puerperal uterine inversion due to submucosal fibroid in a nulliparous woman: a case report. Int J Case Rep Images. 10: 101008Z01JA2019.
- De Vries M, Perquin DA (2010) Non-puerperal uterine inversion due to submucous myoma in a young woman: a case report. J Med Case Rep. 4: 21.
- Karatasli V (2025) Acute non-puerperal uterine inversion caused by a giant uterine leiomyoma with angioleiomyomatous features: a case report. Case Rep Womens Health. 47: e00747.
- Kurniawati EM, Henky AM (2023) A 63-year-old postmenopausal woman with uterine inversion associated with a submucosal Geburt fibroid successfully treated by surgical reversal using the Spinelli procedure. Am J Case Rep. 24: e938390.
- Moshayedi F, Seidaei H, Salehi AM (2022) A case report of non-puerperal uterine inversion due to submucosa leiomyoma in a young virgin woman. Case Rep Surg. 2022: 5240830.
- Bhangale SV, Kumar A, Sharma M, Arora N (2023) A rare case of acute non puerperal complete uterine inversion in nulliparous virgin female. Int J Reprod Contracept Obstet Gynecol. 12: 1908-13.
- Gehlot H, Hemlata, Verma R, Meena GL (2016) Chronic non-puerperal uterine inversion: a rare case report. Int J Reprod Contracept Obstet Gynecol. 5: 1629-32.
- Sofat A, Dubey S, Tandon R, Sehgal A, Aggarwal P (2023) Chronic non-puerperal incomplete uterine inversion. Int J Reprod Contracept Obstet Gynecol. 12: 1902-04.
- Lewin JS, Bryan PJ (1989) MR imaging of uterine inversion. J Comput Assist Tomogr. 13: 357-359.
- Mihmanli V, Kilic F, Pul S, Kilinc A, Kilickaya A (2015) Magnetic resonance imaging of non-puerperal complete uterine inversion. Iran J Radiol. 12: e9878.
- Auber M, Darwish B, Lefebure A, Ness J, Roman H (2011) Management of nonpuerperal uterine inversion using a combined laparoscopic and vaginal approach. Am J Obstet Gynecol. 204: e7-9.

Figures at a glance